St. Louis born rabbi tells his story of working a Covid ICU
Published January 18, 2022
“As a rabbi who works as a chaplain at a hospital in Indianapolis, I’ve held my tongue a lot when it comes to COVID-19 and the emotional strain it puts on the medical staff. But now — as my team at Indiana University Health is responsible for pastoral care in the Medical ICU and its associated unit — is the right time to speak about it.”
That is the quote that St. Louis born Rabbi Mike Harvey used to begin his recent commentary article offering vivid detail of his experience working as a chaplain inside an Indiana hospital. The article created quite a stir amongst local media in Indiana, as well garnering some national coverage.
Rabbi Mike Harvey
Harvey was born in St. Louis in 1981 and attended Craig Elementary School before moving on to MICDS for Middle and High School, graduating in 2000.
At 17, he said he attended a career day event at Shaare Emeth and became interested in becoming a rabbi. Years later, after college, he contacted Rabbi Jeffrey Stiffman, who supported and guided Harvey through his journey.
Early on, Harvey was interested in Clinical Pastoral Education (CPE).
“I did a unit of CPE, required by my seminary (HUC-JIR). In my case, I attended HUC-JIR in Cincinnati, and my Clinical Pastoral Education unit was at Norton Hospital and Kosair Children’s Hospital in Louisville, KY,” remembers Harvey. “Moreover, being a congregational rabbi requires a great deal of pastoral and spiritual care not only for congregants in the hospital but those who come to you with personal issues. That all being said, nothing truly prepares you for what you can and do see as a chaplain.
Here is Harvey’s experience in its entirety.
I am a rabbi in a hospital ICU. This is what the COVID surge looks like to our exhausted staff.
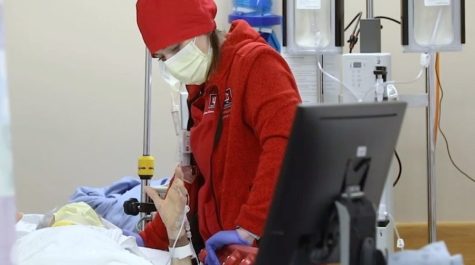
As a rabbi who works as a chaplain at a hospital in Indianapolis, I’ve held my tongue a lot when it comes to COVID-19 and the emotional strain it puts on medical staff. But now — as my team at Indiana University Health is responsible for pastoral care in the Medical ICU and its associated unit — is the right time to speak about it.
My unit is where the sickest of the sick in the state come for care. Our ICU houses patients that other hospitals can’t handle. When it’s a last-ditch effort, they send them to us.
Most of the patients I see in the ICU are COVID-19 positive. Yes, there are other units that hold COVID-positive patients who have less severe symptoms — mainly vaccinated patients with strong working immune systems. Other patients are suffering illnesses unrelated to the coronavirus. But the vast majority on my patient lists are COVID-positive.
What is it like walking down the halls of the pods of the ICU? It’s cold, it’s dark and it’s quiet. The patients are all intubated, hooked up to massive amounts of equipment, with machines breathing for them and feeding them through tubes.
Heavy blankets cover their bodies
Heavy blankets cover their bodies. Some of the machines are so big that you can’t see anything but their legs. Families aren’t around much: It’s dangerous to visit the hospital these days. COVID has spread to the staff, with over 1,000 staff members out statewide. Nurses are overworked, covering two to three patients each – far more than what’s typical in the ICU.
COVID-19 is an especially cruel disease. To those who have overcome adversity, cancer, multiple sclerosis, bone marrow transplants and the like, COVID swoops in and takes them away from their families. They may have finished chemo just months ago, their diabetes was under control, and yes, they did everything right. Many got vaccinated (if they could, as sometimes it’s useless for those with compromised or no immune systems). They overcame great odds, and yet they come to my unit to die.
“Teach us to number our days,” Psalm 90 tells me, “that we may get a heart of wisdom.”
There are far more who come who are unvaccinated.
The numbers don’t lie. We are swarmed with the unvaccinated. Their family members tell us, “He/she was so stubborn.” They tell us, “Well, I’m going to get vaccinated now” (all it took was the death of a loved one). They tell us they didn’t believe “it” was real, referring to a virus that is soon on track to take 6 million lives worldwide.
They tell us to try to pray. Can you imagine? Sitting in my PPE gear, my M95 mask pinching my face, my face shield fogging up, my gloves tight on my hands, I am asked by the unvaccinated wife to pray for an unvaccinated husband as he lays dying.
What prayer is appropriate?
What prayer is appropriate? Prayer in these cases is no substitute for action – preemptive action that would have said louder than any psalm or supplication, “My faith compelled me to appreciate the miracle of vaccination and act on behalf of the elderly and the vulnerable.”
An old Yiddish tale tells of an exhausted Hasid who came running to his rabbi. “Rebbe, help. Take pity. My house is burning.” The rebbe calmed the Hasid. Then, fetching his stick from a corner of the room, he said, “Here take my stick. Run back to your house. Draw circles around it with my stick, each circle some seven handbreadths from the other. At the seventh circle, step back seven handbreadths, then lay my stick down at the east end of the fire. God will help you.”
The Hasid grabbed the stick and started off. “Listen,” the rebbe called after him, “it wouldn’t hurt also to pour water. Yes, in God’s name, pour water. As much water as you can.”
A nurse walks by as I stand in the doorway of another patient. Their family has moved them to comfort care, with a do-not-resuscitate order. There’s nothing else to do. “Was he vaccinated?” I ask.
“I’ve stopped asking,” she says. “Either answer makes me upset.”
As I walk from room to room
As I walk from room to room I think of the words of the Shulchan Aruch, the book that forms the foundation of Jewish law: “One must refrain from putting coins in one’s mouth, lest it’s covered with dried saliva of those afflicted with boils” (Yoreh De’ah 116). The code of Jewish law lists other certain and suspected dangers, including precautions to take in the face of plague, but concludes with this from Rabbi Moshe Isserles: “A person who guards his soul will distance himself from [dangers] and it is prohibited to rely on a miracle in all of these matters.”
Those last words accompany me as I see nurses setting up feeding tubes and ECMO oxygenation machines: “It is prohibited to rely on a miracle in all of these matters.”
Patients are afraid. Families are heartbroken. They cry and argue in the “quiet rooms,” wondering who brought COVID into the house, which aunt refused to get vaccinated and spread the virus that is now is killing the grandfather. There’s guilt, there’s shame, there’s anger.
And then there’s us
Some people drink, some people eat, to cope with what has become a sort of horror show on repeat: When one body is taken out of the room, another patient takes their place. I experience fatigue. At any point in my work day I could close my eyes and go to sleep right where is sit or stand.
“Modeh ani l’fanecha, melech chai v’kayam, shehechezarta bi nishmati, b’chemla raba emunatecha,” I revive myself with the prayer that is traditionally spoken each morning upon waking. “I thank You, living and enduring sovereign, for You have graciously returned my soul within me. Great is Your faithfulness.”
I’ve got to stay awake, provide care for the crying and stressed nurses, provide care for the families, vaccinated and unvaccinated, provide prayer for those dying alone, with only the sound of the machines to accompany them. Why? Because as a Jew I am obligated to do so, as the Torah teaches me: “You shall not stand idly by the blood of another.”
Indeed, people’s lives are in danger. I’ve been at this since August. The doctors and nurses have been at this for years. How they manage I’ll never know. But even a hello and asking how they’re holding up makes a difference. If you know a nurse or doctor, give them a hug, tell them they matter, thank them.
We seem to be fighting a losing battle. People are dying every day. And when we return to our staff meetings we hear the words “surge,” again and again. It’s scary. It’s exhausting.
Gam zeh yaavor, This too shall end. Until then, I remember the words of another sage, F. Scott Fitzgerald: “Tomorrow we will run faster, stretch out our arms farther…. And then one fine morning — So we beat on, boats against the current, borne back ceaselessly into the past.”
Final Thoughts
After his story was published, I asked Rabbi Harvey if his experience made him a better rabbi.
“I’m not sure I’m a better rabbi; in fact, I feel as though I have struggled with more spiritual subjects than ever before. I am, however, a better person. I see the worst of the worst, death and dying, suffering and grief, and I have such a new profound understanding of COVID-19 and its detrimental effects upon not only patients (vaccinated or unvaccinated) but also to their families. This experience has provided me with incredible empathy and helped me work through my frustrations and anger towards the politicization of the disease.”
















